BlueRock Foot & Ankle Center
With Dr. Jason Rockwood
Meet our Foot & Ankle Specialist
Dr. Jason Rockwood DPM
Dr. Jason Rockwood is a board-certified podiatrist with over 20 years of experience, specializing in foot and ankle care at Blue Rock Medicine’s new Foot and Ankle Center. He is dedicated to providing comprehensive care to help patients maintain a healthy and active lifestyle.
Educational Background
Dr. Rockwood earned his DPM from the California College of Podiatric Medicine and holds an MS in Medical Education. His clinical training included prestigious institutions such as Yale New Haven Hospital and Palmetto General Hospital, specializing in foot and ankle trauma and reconstruction.
Professional Experience
Prior to joining Blue Rock Medicine, Dr. Rockwood practiced at Canyon Foot & Ankle in Idaho and successfully led a podiatric practice in New Mexico. He has been involved in educating and training new doctors, enhancing community healthcare.
Specializations and Interests
Dr. Rockwood specializes in deformity correction, lower extremity trauma, and nerve decompression surgery, drawing from his advanced training and extensive research experience. He is passionate about empowering patients through education and is one of the few surgeons offering the Scandinavian Total Ankle Replacement (STAR).
Personal Philosophy
Dr. Rockwood emphasizes patient education and the latest technologies to achieve optimal outcomes. His personal experiences with ankle issues have deepened his empathy and commitment to care.
Personal Life
Dr. Andrew Gibby MD
Dr. Andrew Gibby completed his Interventional Radiology Fellowship training at the Mallinckrodt Radiological Institute at Barnes Jewish Hospital. He completed his radiology residency training at the George Washington University Hospital where he was chief resident, and has written book chapters and numerous research papers. He is credited with helping to create the Gibby-Cvetko Brain Atlas.
Dr. Conrad Gibby MD
Dr. Conrad Gibby completed his fellowship training at Johns Hopkins University. He also trained at Cleveland Clinic and Baylor College of Medicine. He has written numerous research papers. He has a specific interest in functional imaging of the brain, and has presented papers at major medical societies on this topic.
Dr. Thomas Fjeldsted, D.O.
Thomas Fjeldsted, DO graduated in 2016 from Arizona College of Osteopathic Medicine with his medical degree and completed his family medicine residency at Mountain Vista Medical Center in Mesa, AZ in 2019. He is happy to be back in Provo where he completed his undergraduate degree at BYU.
Dr. Fjeldsted chose Family Medicine as a specialty because of the opportunity to address nearly any one of his patient’s needs, whether acute, chronic, or preventive. As a family physician, he works closely with patients and develops a relationship that fosters trust, optimal health, and happiness. His practice philosophy is stay healthy, be happy.
In his free time, Dr. Fjeldsted enjoys spending time with his family, gardening, San Francisco Giants baseball.
Podiatry Services

Sports Injuries
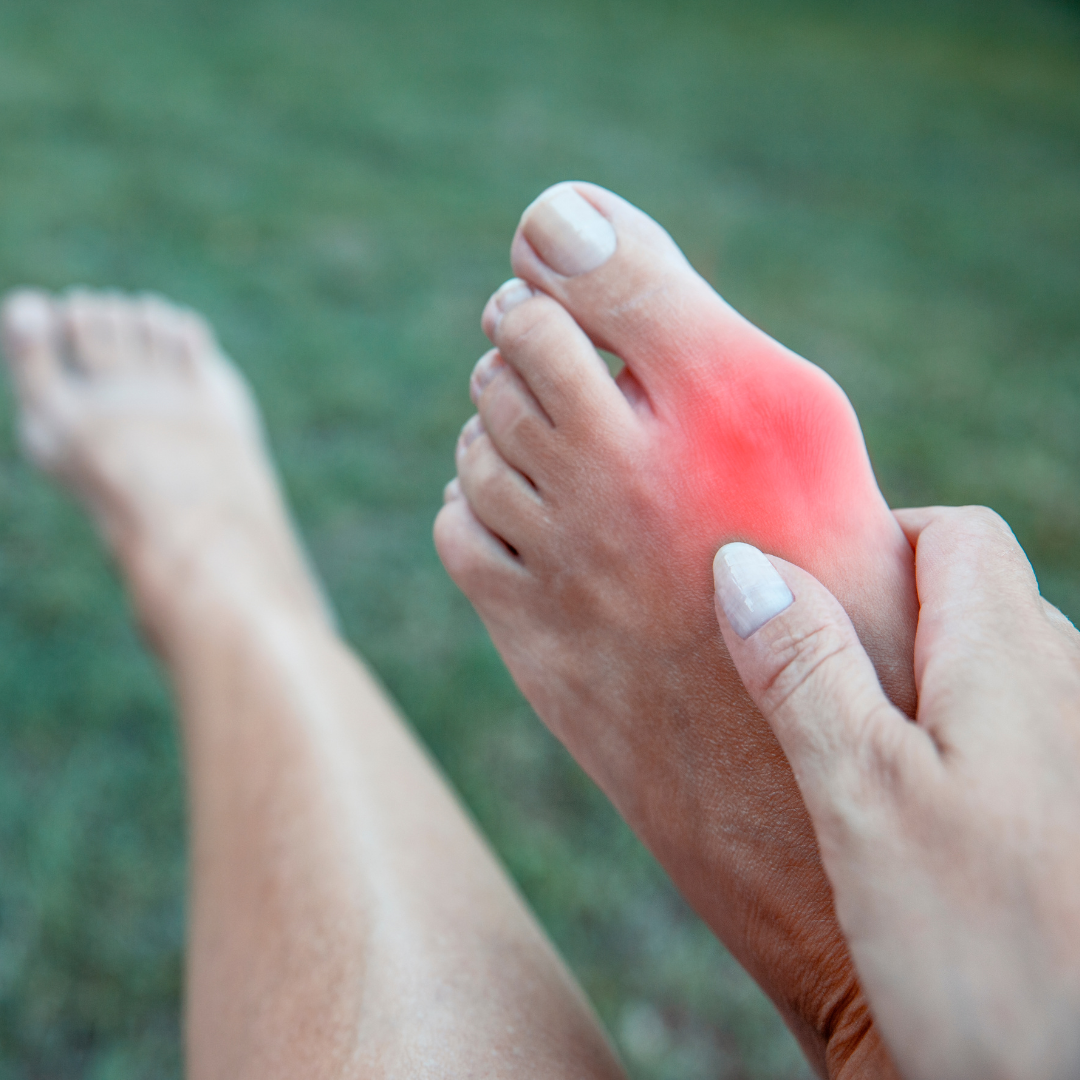
Bunions

Children's Feet

Ball of Foot Pain

Adult-Acquired Flatfoot
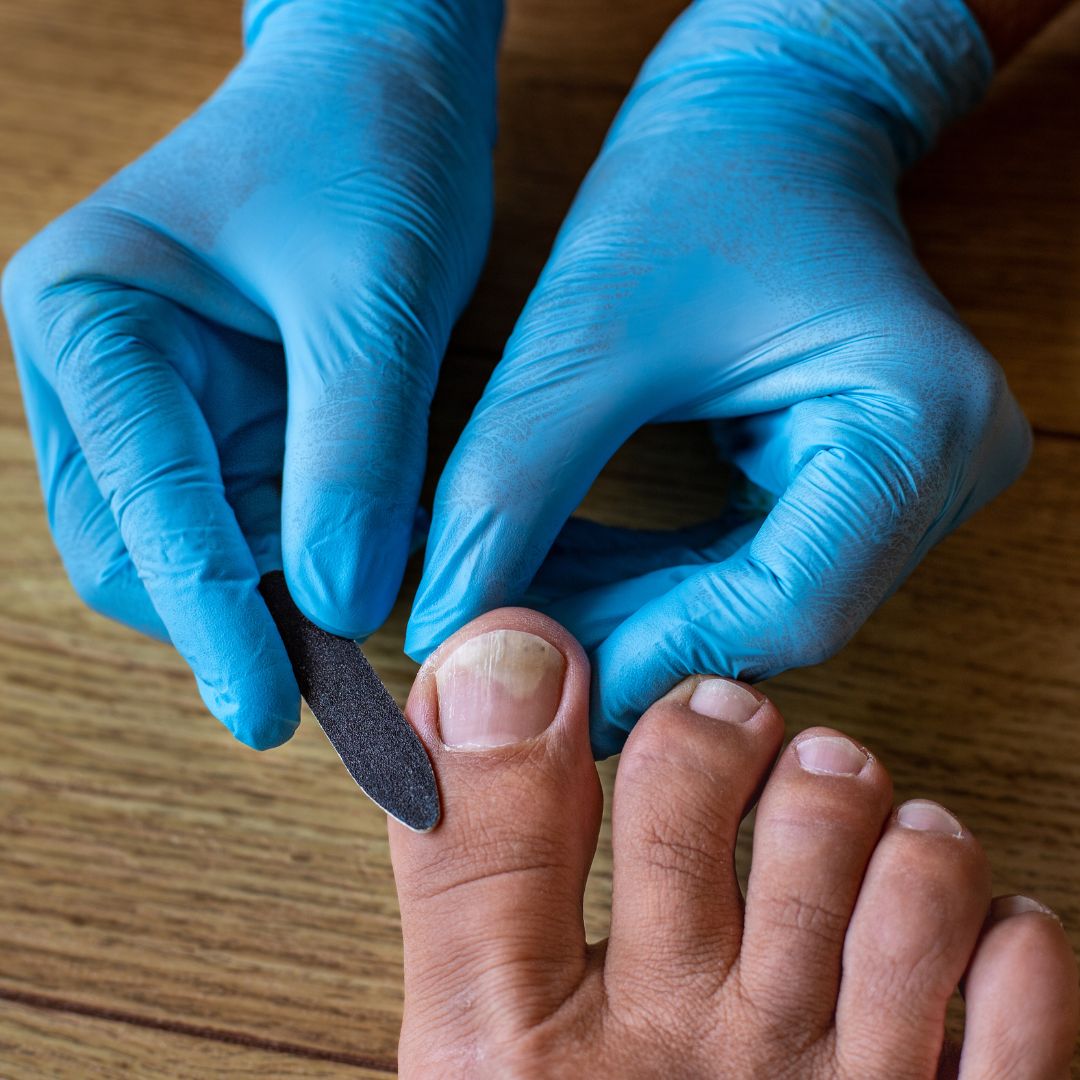
Fungal Toenails

Ankle Sprains

Orthotics
Check and improve your cholesterol levels.

Wart Treatment
Receive help managing your chronic diseases.

Diabetic Foot Care

Ingrown Toenails

Peripheral Neuropathy

Heel Pain

Achilles Tendinitis

Hammertoes

Foot Surgery

Neuromas
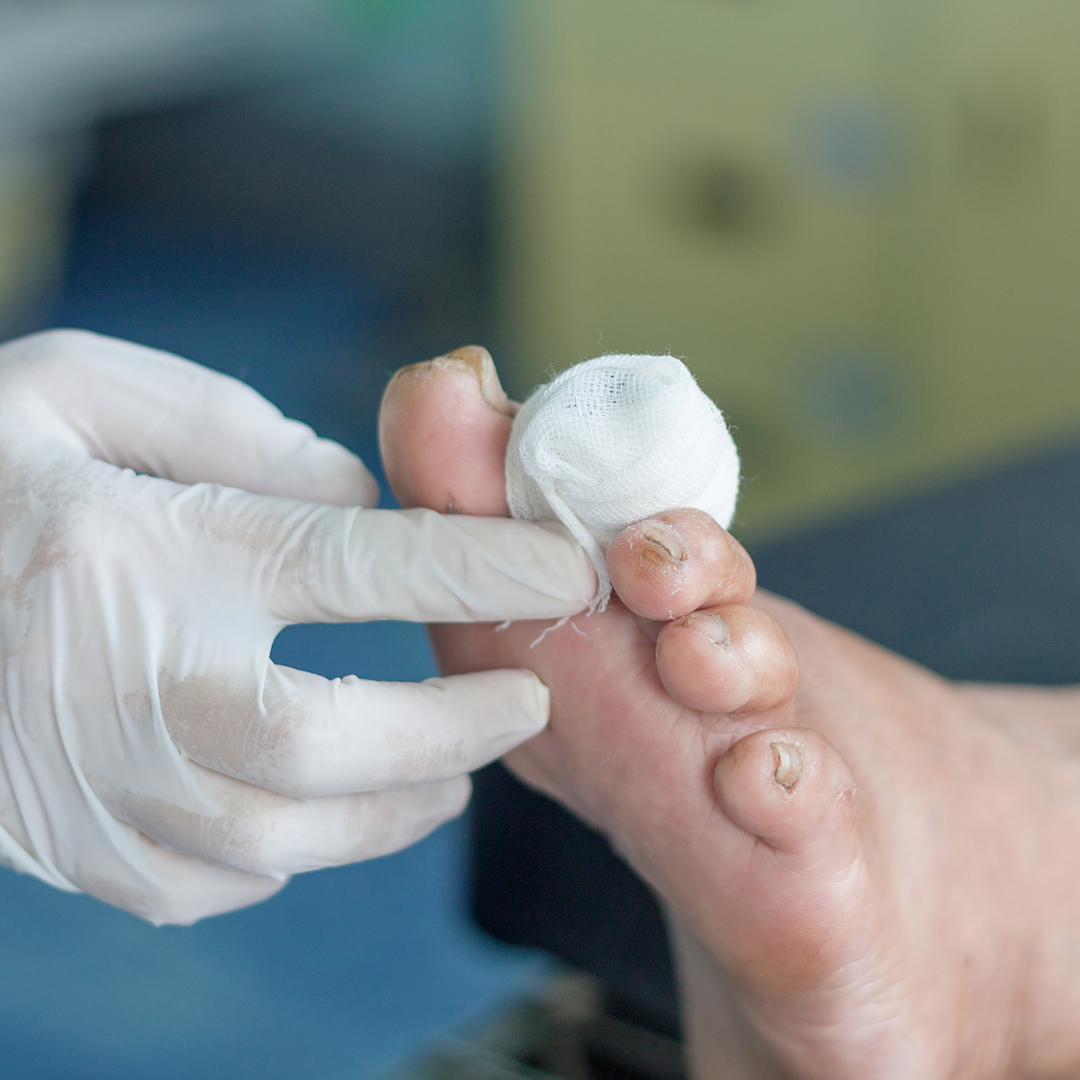
Wound Care

Foot Fractures
Sports-Related Injuries
Understanding Sports-Related Injuries
Sports-related injuries of the foot and ankle are common among athletes and active individuals. These injuries can range from mild sprains to severe fractures and can significantly impact your ability to participate in sports and daily activities.
Symptoms
Common symptoms of sports-related injuries include:
- Pain and tenderness in the affected area
- Swelling and bruising
- Limited range of motion
- Instability or a feeling of the joint giving way
- Difficulty bearing weight on the affected foot or ankle
Diagnosis and Treatment
Accurate diagnosis is crucial for effective treatment. At BlueRock Podiatry, we use advanced imaging techniques, including musculoskeletal ultrasound and MRI, to diagnose sports injuries. Treatment plans are tailored to each patient's needs and may
include non-surgical options like physical therapy and bracing, or surgical interventions when necessary.
At BlueRock Podiatry, we use advanced diagnostic tools to accurately diagnose sports-related injuries, including:
- Physical Examination: Assessing the injury through a thorough physical exam.
- Imaging Tests: X-rays, MRI, and CT scans to visualize the extent of the injury.
- Musculoskeletal Ultrasound: Real-time imaging to evaluate soft tissue injuries.
Common Types of Foot and Ankle Injuries
Ankle Sprains
Description: Ankle sprains occur when the ligaments that support the ankle stretch or tear. They are classified into three grades:
- Grade I: Mild stretching and microscopic tearing of the ligament fibers.
- Grade II: Partial tearing of the ligament.
- Grade III: Complete tear of the ligament.
Achilles Tendon Injuries
Plantar Fasciitis
Stress Fractures
Turf Toe
Peroneal Tendon Injuries
Shin Splints
Treatment Options
We offer a comprehensive approach to treating sports-related injuries, including both non-surgical and surgical options:
Non-Surgical Treatments
- Rest and Ice: Reducing activity and applying ice to decrease inflammation.
- Compression and Elevation: Using a compressive wrap and elevating the foot to reduce swelling.
- Physical Therapy: Exercises to strengthen the muscles and improve flexibility.
- Orthotics: Custom shoe inserts to support the foot and improve alignment.
- Bracing: Ankle braces to provide support and prevent further injury.
- Medications: Anti-inflammatory medications to relieve pain and swelling.
- Injections: Corticosteroid injections to reduce inflammation and pain.
Surgical Treatments
In severe cases where non-surgical treatments are not effective, surgery may be necessary to repair or reconstruct damaged tissues. Surgical options include:
- Ligament Repair
- Tendon Repair
- Fracture Fixation
- Arthroscopy
Prevention Tips
To prevent sports-related injuries, consider the following tips:
Heel Pain
Heel pain is a widespread issue affecting millions of individuals worldwide. It can significantly impact daily activities and overall quality of life. The heel is a crucial structure in the human body, absorbing shock and providing support during walking and running.
Heel pain can result from a variety of conditions, each with its own set of causes and symptoms.
Plantar fasciitis is perhaps the most well-known cause of heel pain, characterized by inflammation of the plantar fascia—a thick band of tissue running across the bottom of the foot from the heel to the toes. This condition often presents as a sharp, stabbing pain in the heel, particularly with the first steps in the morning.
However, plantar fasciitis is not the only source of heel pain. Other common conditions include heel spur syndrome, infracalcaneal bursitis, and heel pad syndrome, a condition affecting the fatty tissue in the heel.
Causes
Heel pain can also be due to neurological conditions such as tarsal tunnel syndrome, Baxter’s neuritis, and nerve entrapment, leading to nerve-related pain and symptoms.
Other factors contributing to heel pain include flat-feet, high arches and occupational hazards. Pregnancy can also lead to heel pain due to increased weight and changes in gait.
For runners and athletes, heel pain is often related to overuse injuries, improper footwear, and biomechanical issues. Conditions such as stress fractures are common in this group, resulting from
repetitive stress on the heel bone.
Accurate diagnosis is essential for effective treatment of heel pain. Evaluations often include clinical assessments, radiological imaging such as X-rays and MRIs, and diagnostic ultrasound to pinpoint the exact cause of pain.
Heel pain, particularly plantar fasciitis, is a common issue that affects a significant portion of the population. Here are some statistics and information on its impact:
Common and Uncommon Sources of Heel Pain
Plantar Fasciitis
- Heel Spur Syndrome
- Infracalcaneal Bursitis
- Heel Pad Syndrome
- Insertional Achilles Tendinitis
- Retrocalcaneal Bursitis
- Tarsal Tunnel Syndrome
- Baxter’s Neuritis
- Stone Bruise
- Nerve Entrapment
- Flatfeet (Overpronation)
- High Arches
- Obesity
- Occupational Hazards
- Pregnancy
- Calcaneal Stress Fracture
Symptoms of Heel Pain
Heel pain can manifest in various ways, with symptoms ranging from mild discomfort to severe, debilitating pain. Understanding these symptoms is crucial for accurate diagnosis and effective treatment.
Sharp Pain, Swelling, Stiffness, Numbness or Tingling, Difficulty Walking or Running, Localized Tenderness, Radiating Pain, Pain with Activity, Achilles tendonitis, and Chronic Discomfort.
Understanding these symptoms and their potential causes is essential for pinpointing the exact condition and developing an effective treatment plan. Accurate symptom assessment can lead to better outcomes and faster relief from heel pain.
Diagnosis of Heel Pain
Accurate diagnosis of heel pain is crucial for effective treatment. The process typically involves a combination of patient history, physical examination, and imaging studies.
Heel pain can arise from various conditions, and not all heel pain is due to plantar fasciitis. It is essential to receive an accurate diagnosis before pursuing treatment. At BlueRock Podiatry, our board-certified doctors are dedicated to helping patients determine the best approach for their heel
pain. We utilize a comprehensive evaluation process to identify the underlying cause and develop a tailored treatment plan that addresses individual needs.
If you are experiencing heel pain, don’t hesitate to reach out to BlueRock Podiatry. Our team is here to help you find relief and get back to your daily activities.
Illness Treatment
Fungal Toenails
Call 801-356-0233 to schedule an appointment today!
Ingrown Toenails
Ingrown toenails occur when the edges of the toenail grow into the surrounding skin, leading to discomfort, redness, and swelling. While it may sound concerning, the good news is that ingrown toenails are easily treatable, and our experienced team is here to help!
Look for the following signs:
- Pain or tenderness along the edge of the toenail
- Redness and swelling around the nail
- Possible drainage of fluid or pus
If you notice these symptoms, it’s important to take action. While some mild cases can be managed at home, it’s always best to consult a professional for a proper diagnosis and treatment plan.
**Important**:
If you or your child have reduced sensation in your feet, or if you are soaking a child’s feet, always check the water temperature with your hand before soaking to prevent burns.
Additionally, we generally recommend that patients with diabetes and neuropathy avoid
soaking until they have been seen by a doctor.
What to Avoid While at-home
There are certain things you should avoid to prevent worsening the condition:
- Do Not Dig or Pick
- Avoid Tight Footwear
Don’t Ignore Symptoms
If symptoms persist or worsen, seek professional help rather than trying to manage the condition on your own.
Why See an Experienced Podiatrist?
While at-home care can provide temporary relief, seeing an experienced podiatrist is crucial for effective treatment. Our specialists have the knowledge and skills to assess the severity of the ingrown toenail and recommend the best course of action. Ignoring the issue can lead to complications, including infections or chronic pain.
Treatment Options
At our podiatry office, we offer a range of treatment options tailored to your needs, addressing both acute and chronic ingrown toenails:
Temporary Solutions: For acute cases, we may recommend:
- Antibiotics
- Pain-Free Nail Trimming
Permanent Solutions for chronic ingrown toenails:
- Minor Procedures with Anesthesia
- Nail Matrix Removal
Don’t let ingrown toenails disrupt your life or your child’s activities. Contact us today to schedule an appointment and take the first step towards comfortable, healthy feet!
Neuromas
Understanding Foot Neuromas
Foot neuromas, also known as Morton’s neuromas, are a painful condition affecting the nerves between the toes. Despite the name, a neuroma is not actually a tumor or growth; rather, it is an inflammation of the digital nerve, most commonly occurring between the third and fourth digits on the bottom of the foot. This condition often results from nerve compression or irritation, leading to pain, tingling, and numbness in the affected area. Understanding the causes, symptoms, diagnosis, and treatment options for neuromas is essential for effective management and relief.
What is a Neuroma?
A neuroma is a benign growth of nerve tissue, most commonly occurring between the third and fourth toes. This condition leads to pain and discomfort, especially when walking or wearing tight shoes.
Causes
- Foot Structure: Flat feet, high arches, or other anatomical abnormalities that increase pressure on the forefoot.
- Footwear: Tight, narrow, or high-heeled shoes that compress the toes and forefoot.
- Activities: High-impact activities that put repetitive stress on the feet, such as running or jumping.
- Injury: Trauma or injury to the foot can lead to the development of a neuroma.
- Other Conditions: Conditions like bunions or hammertoes that alter the foot's structure and increase nerve pressure.
Symptoms
- Pain: Sharp, burning pain in the ball of the foot, often radiating to the toes.
- Tingling and Numbness: Tingling or numbness in the affected toes.
- Swelling: Swelling between the toes.
- A "Pebble" Sensation: Feeling like there is a pebble or lump in your shoe.
- Worsening with Activity: Symptoms typically worsen with walking, running, or wearing tight shoes.
Diagnosis
Clinical Evaluation
- Patient History: Understanding the onset, duration, and characteristics of the symptoms.
- Physical Examination: Inspecting for tenderness, swelling, and abnormal foot structures.
- Palpation: Feeling for a palpable mass or "click" between the toes.
- Special Tests: Performing tests like the Mulder’s sign to identify nerve compression.
Imaging Studies
- X-rays: To rule out other conditions like fractures or arthritis.
- Ultrasound: To visualize the neuroma and assess soft tissue structures.
- MRI: To provide detailed images of the neuroma and surrounding tissues.
Treatment Options
Non-Surgical Treatments
- Footwear Modification: Wearing shoes with a wide toe box and good arch support to reduce pressure on the neuroma.
- Padding and Orthotics: Using metatarsal pads or custom orthotics to relieve pressure on the nerve.
- Activity Modification: Reducing high-impact activities that exacerbate symptoms.
- Medications: NSAIDs to reduce pain and inflammation.
- Physical Therapy: Exercises to strengthen and support the foot.
- Injections: Corticosteroid injections to reduce inflammation around the nerve.
Surgical Treatments
- Decompression vs. Neurectomy: When conservative treatments fail, surgery may be considered for Morton's neuroma. There are two main surgical options: decompression and neurectomy.
- Decompression: This procedure involves releasing the pressure on the nerve by cutting the ligaments or other structures compressing it. The goal is to preserve the nerve while alleviating symptoms. Decompression is often preferred for patients who wish to maintain sensation in the affected area.
- Neurectomy: This involves removing the affected nerve segment. Neurectomy is typically considered when decompression is not effective or when the neuroma is particularly large. However, this procedure may result in permanent numbness in the area supplied by the nerve.
The choice between decompression and neurectomy depends on several factors, including the size and location of the neuroma, the patient's symptoms, and their personal preferences. Recent research suggests that both procedures can be effective, but decompression may offer a better quality of life for some patients by preserving nerve function.
- Cryogenic Neuroablation: Freezing the nerve to relieve pain.
Recovery and Rehabilitation
- Rest: Adequate rest to allow for healing.
- Gradual Return to Activity: Slowly increasing activity levels as symptoms improve.
- Exercises: Specific exercises to strengthen the foot and improve flexibility.
- Monitoring: Regular follow-ups to monitor progress and adjust the treatment plan as needed.
Prevention
- Proper Footwear: Wearing supportive, well-fitted shoes with a wide toe box.
- Avoiding High Heels: Limiting the use of high-heeled shoes.
- Safe Practices: Using proper techniques in sports and exercise to avoid excessive stress on the feet.
- Foot Health Maintenance: Regularly stretching and strengthening foot muscles.
Foot neuromas can be a painful and debilitating condition, but with proper diagnosis, treatment, and preventive measures, most people can achieve significant relief. At BlueRock Podiatry, our expert team is equipped to provide comprehensive care for foot neuromas, utilizing advanced diagnostic tools and personalized treatment plans to ensure optimal outcomes.
Foot Fractures
Foot fractures are common injuries that can affect any of the bones in the foot. These
fractures can range from tiny cracks in the bone, known as stress fractures, to complete
breaks that can cause severe pain and disability. At BlueRock Podiatry, part of BlueRock Medical Center, you can avoid the long wait at the ER and be seen same-day for most injuries by board-certified foot and ankle surgeons. Understanding the causes, symptoms, diagnosis, and treatment options for foot fractures is essential for proper management and recovery.
Types of Foot Fractures
1. Stress Fractures: Small cracks in the bone caused by repetitive force or overuse. Common in athletes and those with high-impact activities.
2. Traumatic Fractures: Complete or partial breaks caused by a direct blow or impact, such as from an accident or heavy object dropping on the foot.
3. Avulsion Fractures: When a fragment of bone is pulled off by a tendon or ligament due to a sudden force.
4. Displaced vs. Non-displaced Fractures
o Displaced: Bone fragments are misaligned, often requiring surgical
intervention.
o Non-displaced: Bone fragments remain in proper alignment and can often
be treated non-surgically.
Common Causes
Sports Injuries: High-impact sports or activities that place stress on the foot.
Accidents: Falls, collisions, or dropping heavy objects on the foot.
Overuse: Repetitive stress from activities like running or jumping.
Osteoporosis: Weakening of the bones making them more susceptible to fractures.
Improper Footwear: Lack of support or wearing worn-out shoes that fail to protect
the feet adequately.
Symptoms
Pain: Immediate and intense pain at the site of the fracture, which may worsen with
movement.
Swelling: Swelling around the affected area, often accompanied by bruising.
Bruising: Discoloration and bruising around the fracture site.
Deformity: Visible deformity in case of displaced fractures, where the bone
fragments are out of alignment.
Difficulty Walking: Inability to bear weight or walk on the affected foot due to pain and instability.
At BlueRock Podiatry, we utilize state-of-the-art imaging technology to ensure accurate and comprehensive diagnosis of foot fractures.
Foot fractures can be debilitating, but with proper diagnosis, treatment, and rehabilitation, most people can recover fully. At BlueRock Podiatry, our expert team and state-of-the-art imaging technology ensure that you receive the best care for your foot fractures. If you suspect a foot fracture, seek medical attention promptly to ensure proper management and prevent complications.
Peripheral Neuropathy
Understanding Diabetic Peripheral Neuropathy: A Focus on Lower Extremity Health
Welcome to our resource on Diabetic Peripheral Neuropathy (DPN), a condition that affects many individuals with diabetes, particularly in the lower extremities. As a podiatrist, I am dedicated to helping you understand this condition and the various treatment options available to improve your foot health and overall quality of life.
What is Diabetic Peripheral Neuropathy?
Diabetic Peripheral Neuropathy is a type of nerve damage that occurs as a result of prolonged high blood sugar levels in individuals with diabetes. It primarily affects the peripheral nerves, which are responsible for transmitting signals between the brain and the rest of the body. When these nerves are damaged, it can lead to a range of symptoms, particularly in the feet and legs.
How Does DPN Affect the Lower Extremities?
In the lower extremities, DPN can manifest in several ways:
- Numbness and Tingling: Many patients report a "pins and needles" sensation in their feet, which can progress to complete numbness.
- Pain: Some individuals experience sharp, burning, or aching pain, which can be debilitating.
- Weakness: Muscle weakness may occur, leading to difficulty walking or maintaining balance.
- Loss of Reflexes: DPN can affect the body's ability to respond to stimuli, increasing the risk of falls and injuries.
- Foot Ulcers and Infections: Reduced sensation can lead to unnoticed injuries, increasing the risk of ulcers and infections.
Treatment Options for Diabetic Peripheral Neuropathy
Fortunately, there are several treatment options available to manage the symptoms of DPN and improve foot health. Here’s a broad but specific list of treatments
1. Lifestyle Modifications
- Blood Sugar Control: Maintaining optimal blood glucose levels is crucial in preventing further nerve damage.
- Dietary Changes: A balanced diet rich in whole grains, lean proteins, and healthy fats can support overall health.
- Regular Exercise: Engaging in regular physical activity can improve circulation and nerve function.
2. Medications
- Pain Relievers: Over-the-counter pain medications may help alleviate mild discomfort.
- Antidepressants: Certain antidepressants, such as Duloxetine and Amitriptyline, can be effective in managing neuropathic pain.
- Anticonvulsants: Medications like Gabapentin and Pregabalin are often prescribed to reduce nerve pain.
3. Topical Treatments
- Capsaicin Cream: This topical treatment can help reduce pain by desensitizing nerve endings.
- Lidocaine Patches: These patches can provide localized pain relief.
4. Physical Therapy
- A physical therapist can design a personalized exercise program to improve strength, flexibility, and balance.
5. Foot Care
- Regular foot inspections and proper footwear are essential to prevent injuries and complications.
- Podiatrists can provide specialized foot care and treatment for any existing foot problems.
6. Decompression Nerve Surgery
What is it? Decompression nerve surgery is a procedure designed to relieve pressure on nerves that may be contributing to neuropathic pain and other symptoms associated with DPN.
Indications for Surgery:
- Patients with significant pain or functional impairment that has not improved with conservative treatments.
- Conditions such as tarsal tunnel syndrome, where the posterior tibial nerve is compressed at the ankle.
Procedure Overview:
- The surgery involves making a small incision to access the affected nerve and removing any structures that may be causing compression.
- The goal is to restore normal nerve function and alleviate symptoms.
7. Alternative Therapies
- Some patients find relief through acupuncture, massage therapy, or other complementary treatments.
Diabetic Peripheral Neuropathy can significantly impact your quality of life, especially when it affects the lower extremities. However, with the right treatment plan and proactive foot care, you can manage your symptoms and maintain your mobility. If you are experiencing symptoms of DPN or have concerns about your foot health, please don’t hesitate to reach out for a consultation. Together, we can develop a personalized approach to improve your foot health and overall well-being.
Ball of Foot Pain
Ball of foot pain, is a common issue. The ball of the foot, located just behind the toes, is a crucial area that bears much of our body weight during activities like walking, running, and standing. When pain occurs in this area, it can significantly impact your daily life. In this guide, we will explore the most common conditions that cause pain in the ball of the foot, helping you understand the symptoms, causes, and treatment options available.
Common Conditions Affecting the Ball of the Foot
Morton's Neuroma
Morton's neuroma is a thickening of the tissue around a nerve leading to the toes, often between the third and fourth toes. This condition can cause sharp, burning pain in the ball of the foot, along with tingling or numbness in the toes. It is commonly aggravated by tight shoes or high heels.
Metatarsophalangeal Joint Capsulitis
Capsulitis is an inflammation of the ligaments surrounding the metatarsophalangeal (MTP) joints, which connect the toes to the foot. This condition can lead to pain and swelling in the ball of the foot, particularly during activities that involve pushing off the toes.
Injury to the Plantar Plate
The plantar plate is a thick ligament that supports the MTP joints. An injury or tear to this structure can cause pain in the ball of the foot, often accompanied by swelling and difficulty walking. This condition is more common in athletes and individuals who engage in high-impact activities.
Loss of Fat Pad
As we age, the natural fat pad that cushions the ball of the foot can thin out, leading to increased pressure and pain. This condition can make walking uncomfortable and may require adjustments in footwear.
Contractures of the Digits
Contractures occur when the toes bend abnormally, often due to muscle imbalances or conditions like arthritis. This can lead to pain in the joints of the toes and the ball of the foot, making it difficult to find comfortable footwear.
Stress Fractures of the Metatarsals
Stress fractures are small cracks in the bones of the foot, often caused by repetitive stress or overuse. They can lead to localized pain in the ball of the foot, especially during weight-bearing activities.
Sesamoiditis
Sesamoiditis is an inflammation of the sesamoid bones, which are small bones located beneath the big toe joint. This condition can cause pain under the big toe joint, particularly during activities that involve pushing off, such as running or jumping.
When to Seek Help
If you are experiencing persistent pain in the ball of your foot that interferes with your daily activities, consult a healthcare professional. Early diagnosis and treatment can help prevent further complications and improve your quality of life.
Visit Us!
Ball of foot pain can arise from various conditions, each requiring a tailored approach to treatment. Take proactive steps to manage your foot health. Find personalized care and effective treatment options at BlueRock Podiatry.
Treating Foot Warts
Warts are small, noncancerous growths on the skin caused by the human papillomavirus (HPV). There are more than 100 types of HPV, and different types of the virus can cause warts to appear on different parts of the body. Warts are generally harmless but can be bothersome and sometimes painful.
Causes of Warts
Warts are caused by an infection with HPV. The virus enters the skin through tiny cuts or breaks. It then causes the top layer of skin to grow rapidly, creating a wart. The virus is more likely to infect the skin if it is cut or damaged in some way.
Why Feet Are Prone to Warts
The feet are particularly prone to warts, known as plantar warts, because they often come into contact with environments where the virus can thrive, such as communal showers, locker rooms, and swimming pools. The warm, moist environment of shoes and socks can also encourage the growth of warts. Furthermore, the pressure and friction from walking or standing can cause the virus to penetrate the skin more easily.
Difference Between a Wart and a Plantar Wart
Warts: These can appear anywhere on the body. They are usually rough, hard bumps that may have black dots (wart seeds).
Plantar Warts: These specifically occur on the soles of the feet. Unlike common warts that grow outward, plantar warts tend to grow inward due to the pressure from walking, making them flat and sometimes painful. They can be mistaken for calluses.
What Do Warts Look Like and Feel Like?
Appearance: Warts can be flesh-colored, dark pink, yellow, brown, purple, or gray. They may have a rough texture and small black dots, which are tiny blood vessels that have clotted.
Feel: Warts can feel rough and hard, like a small bump. Plantar warts can feel particularly painful when pressure is applied, such as while walking.
Why Are Some Warts Painful and Some Not?
Warts can be painful if they grow in areas where pressure is frequently applied, such as the soles of the feet. This pressure pushes the wart inward, which can cause pain. Warts on less pressure-prone areas of the body are usually painless unless they grow large.
Visit Our Foot & Ankle Center
Dr. Jason Rockwood provides personalized care for all your foot and ankle needs. With extensive training and experience, we offer the latest treatments and techniques to help you manage and treat warts effectively.
Contact Us
If you're experiencing symptoms of warts, don't wait to seek treatment. Contact BlueRock Podiatry today to schedule an appointment and start your journey to recovery.
Pelvic Congestive
How is pelvic congestion syndrome treated?
Gonadal vein embolization is a minimally invasive treatment for pelvic congestion syndrome. The goal is to close off faulty veins so they can no longer enlarge with blood, thus relieving pain and symptoms of pelvic congestion syndrome.
Hammertoes
Understanding Hammertoes
Hammertoes are a common foot problem where the toes become bent at the middle joint, causing them to resemble a hammer. This condition can be painful and can make it difficult to wear certain types of shoes and perform everyday activities.
Symptoms
Common symptoms of hammertoes include:
- Pain and discomfort in the affected toes
- Corns or calluses on the top of the toe joint
- Swelling and redness around the toe
- Difficulty moving the affected toe
- Pain when wearing shoes
Causes
Hammertoes can be caused by:
- Footwear Choices: Tight, narrow shoes or high heels that push the toes into a bent position.
- Genetic Factors: Inherited foot structure abnormalities.
- Muscle Imbalance: Weak or tight muscles in the foot.
- Underlying Medical Conditions: Arthritis, diabetes, or nerve damage.
Treatment Options
At BlueRock Podiatry, we offer a comprehensive approach to treating hammertoes, including both non-surgical and surgical options:
Non-Surgical Treatments
- Footwear Modifications
- Orthotics
- Padding and Taping
- Toe Exercises
- Splinting and Bracing
- Medications
- Shockwave Therapy
Surgical Treatments
In cases where non-surgical treatments are not effective, surgical options may be considered, including:
- Soft Tissue Release: Releasing tight tendons and ligaments to allow the toe to move back into its natural position.
- Tendon Transfer: Repositioning tendons to correct the alignment of the toe.
- Bone Realignment: Surgically realigning the bones of the toe to correct the deformity.
- Minimally Invasive Surgery: Techniques that involve smaller incisions and less soft tissue disruption, leading to faster recovery times³.
Risks and Benefits of Surgical Options
Soft Tissue Release and Tendon Transfer
Benefits:
- Corrects the toe alignment
- Reduces pain and discomfort
- Improves foot function
Bone Realignment and Minimally Invasive Surgery
Benefits:
- Provides a more permanent correction
- Minimally invasive options reduce recovery time
- Less postoperative pain and swelling
Risks:
- Risk of incomplete correction
- Potential for infection or nerve damage
- Longer recovery time for traditional bone realignment
Prevention Tips
To prevent hammertoes, consider the following tips:
- Choose shoes with a wide toe box and good arch support
- Avoid high heels and narrow, pointed shoes
- Perform regular foot exercises to strengthen the muscles
- Monitor for any changes in toe alignment and seek early treatment
Why Choose BlueRock Podiatry?
The team at BlueRock Podiatry is dedicated to providing personalized care for all your foot and ankle needs. With extensive training and experience, we offer the latest treatments and techniques to help you manage hammertoes effectively and improve your quality of life.
MLS Laser Therapy
Manage Pain.
Reduce Inflammation.
Speed Recovery.
What is Laser Therapy?
Laser Therapy is the use of specific wavelengths of light to treat painful and debilitating conditions.
How does it work?
Light energy enters the damaged cells and stimulates inter-cellular activity. This reduces pain in the area and speeds the recovery of the damaged cells. Once the cells recover, the healing process is complete.
What can I expect during a treatment?
MLS Laser Therapy is a painless treatment that lasts an average of 8 minutes. You may experience a comfortable sensation at the point of application.
What can I expect after the treatment?
Most people experience positive results in 1 to 3 treatments, with the average course of treatment being 7 to 10 sessions. Swelling is greatly reduced and there is a rapid relief of pain. Acute conditions usually subside quickly, typically within one phase of treatments, while chronic conditions can be controlled with regular treatments.
The effects of MLS Laser Therapy are cumulative; therefore, expect to see improvement as you proceed through your treatment plan. It is critical that once you start, you complete the course of treatments recommended by your doctor or symptoms are likely to reoccur.
MLS Laser Therapy effectively treats:
- Tendon & ligament injuries
- Sore muscles, muscle strains & tears
- Degenerative joint conditions
- Neurological & general pain & bruising
- Musculoskeletal disorders
- Pre & post-surgical treatment
- Anti-inflammation applications
- Specific neurological conditions
Benefits of MLS Laser Therapy
- Rapid relief of pain
- Strong anti-inflammatory effect
- Timely healing of sprains & strains
- Rapid recovery of the structural integrity of the injured region.
- Rapid resolution of swollen areas
- Immediate improvement of local blood circulation
- Rapid repair of superficial injuries, such as wounds and ulcers.
Bunions
Understanding Bunions
A bunion is a bony bump that forms on the joint at the base of your big toe. It occurs when some of the bones in the front part of your foot move out of place, causing the tip of your big toe to get pulled toward the smaller toes and forcing the joint at the base of your big toe to stick out. This can lead to pain and discomfort, especially when wearing shoes.
Symptoms
Common symptoms of bunions include:
- A bulging bump on the outside of the base of your big toe
- Swelling, redness, or soreness around your big toe joint
- Corns or calluses where the first and second toes overlap
- Persistent or intermittent pain
- Restricted movement of your big toe
Causes
Bunions can be caused by:
- Inherited foot type
- Foot injuries
- Deformities present at birth
- Wearing tight, narrow shoes
- Combination of above factors
Treatment Options
At BlueRock Podiatry, we offer a comprehensive approach to treating bunions and related forefoot pain, including both non-surgical and surgical options:
Non-Surgical Treatments
- Footwear Modifications: Wear shoes with a wide toe box to reduce pressure on the bunion.
- Orthotics: Custom shoe inserts to support the foot and improve alignment.
- Padding and Taping: Protecting the bunion and reducing pain.
- Medications: Anti-inflammatory medications to relieve pain and swelling.
- Physical Therapy: Exercises to strengthen the muscles around the foot and improve flexibility.
Surgical Treatments
In cases where non-surgical treatments are not effective, surgical options may be considered, including:
Traditional Bunionectomy: Removing the swollen tissue around your big toe joint and realigning the bone with combination of different bone cuts (osteotomies) and fixation with plates and screws when necessary.
Lapidus Bunionectomy: A surgical procedure that involves fusing the first metatarsal bone to the medial cuneiform bone to correct the bunion and stabilize the joint. This technique addresses the bunion in all three planes and is particularly effective for severe deformities.
Percutaneous Bunion Procedures: Minimally invasive techniques that involve smaller incisions and less soft tissue disruption. These procedures can reduce recovery time and postoperative pain.
Prevention Tips
To prevent bunions and related forefoot pain, consider the following tips:
- Choose shoes with a wide toe box and good arch support
- Avoid high heels and narrow, pointed shoes
- Maintain a healthy weight to reduce stress on your feet
- Perform regular foot exercises to strengthen the muscles
Why Choose BlueRock Podiatry?
The team at BlueRock Podiatry is dedicated to providing personalized care for all your foot and ankle needs. With extensive training and experience, we offer the latest treatments and techniques to help you manage bunions effectively and improve your quality of life.
Ankle Sprains
Ankle Sprains, Instability, and Peroneal Tendon Injuries
Ankle sprains are common injuries that occur when the ligaments supporting the ankle stretch or tear. Repeated ankle sprains can lead to chronic ankle instability, characterized by a persistent feeling of the ankle giving way.
Symptoms
Common symptoms of ankle sprains and instability include:
- Pain and swelling around the ankle
- Bruising
- Difficulty bearing weight
- A feeling of instability or the ankle giving out
Causes
Ankle sprains and instability can be caused by:
- Sudden twisting or rolling of the ankle
- Previous ankle injuries
- Weakness in the muscles surrounding the ankle
- Loose or overstretched ligaments
Peroneal Tendon Injuries
Peroneal tendon injuries, including tears and split tears, often occur alongside ankle sprains and instability. The peroneal tendons run along the outside of the ankle and help stabilize the foot.
Types of Peroneal Tendon Injuries
- Tendonitis: Inflammation of the tendons due to overuse.
- Tears: Partial or complete tears of the tendons, often resulting from acute trauma or chronic overuse.
- Split Tears: Longitudinal tears in the tendon, commonly seen in the peroneus brevis tendon.
Diagnosis
Accurate diagnosis is crucial for effective treatment. At BlueRock Podiatry, we use a combination of musculoskeletal ultrasound and MRI to diagnose ankle sprains, instability, and peroneal tendon injuries. Ultrasound provides real-time imaging of the tendons and ligaments.
Treatment
Non-Surgical Treatments
- Rest and Ice: Reducing activity and applying ice to decrease inflammation.
- Physical Therapy: Exercises to strengthen the muscles around the ankle and improve stability.
- Bracing: Ankle braces to support the foot and prevent further injury.
- Medications: Anti-inflammatory medications to relieve pain and swelling.
Surgical Treatments
In cases where non-surgical treatments are ineffective, surgery may be necessary to repair damaged ligaments and tendons and stabilize the ankle.
Arthroscopy with Debridement
Arthroscopy with debridement is a minimally invasive surgical procedure that involves using a small camera (arthroscope) to visualize the inside of the ankle joint and remove damaged tissue or bone spurs.
Combined Diagnostic and Therapeutic Debridement
This procedure involves both diagnosing and treating issues within the ankle joint. It allows for a thorough examination and immediate treatment of any identified problems.
Surgical Repair of Peroneal Split Tear
Surgical repair of a peroneal split tear involves identifying and repairing the damaged tendon to restore its function and alleviate pain.
Internal Brace Device for Ankle Stabilization
One advanced surgical option for repairing ankle instability is the use of an internal brace device, such as those from Arthrex. This technique involves augmenting the primary ligament repair with a strong, flexible brace that provides additional support during the healing process.
Work with your doctor to determine which option is best for you!
Why Choose BlueRock Podiatry?
The team at BlueRock Podiatry is dedicated to providing personalized care for all your foot and ankle needs. With extensive training and experience, we offer the latest treatments and techniques to help you recover quickly and return to your active lifestyle.
Contact Us
If you're experiencing symptoms of ankle sprains, instability, or peroneal tendon injuries, don't wait to seek treatment. Contact BlueRock Podiatry today to schedule an appointment and start your journey to recovery.
Children's Feet
Understanding Children's Foot Health:
Common Conditions and Care
Welcome to our comprehensive guide on children's foot health! As parents, it's essential to understand the common foot problems that children may experience as they grow. Healthy feet are crucial for your child's overall development, mobility, and confidence. In this guide, we will explore various foot conditions, their symptoms, causes, and treatment options, ensuring you have the knowledge to support your child's foot health.
Achilles Tendinitis
What is Achilles Tendonitis?
Achilles tendonitis is a common condition that affects the Achilles tendon, the band of tissue that connects your calf muscles to your heel bone. This condition is often caused by overuse or intense strain on the tendon, leading to inflammation and pain.
Symptoms
Common symptoms of Achilles tendonitis include:
- Pain and stiffness along the Achilles tendon, especially in the morning
- Swelling in the back of your heel
- Limited range of motion when flexing your foot
- A feeling of warmth over the affected area
Causes
Achilles tendonitis can be caused by:
- Sudden increase in the intensity or duration of physical activity
- Tight calf muscles
- Bone spurs
- Wearing improper footwear
- Running on hard surfaces
Treatment Options
At BlueRock Podiatry, we offer a comprehensive approach to treating Achilles tendonitis, including both non-surgical and surgical options:
Non-Surgical Treatments
- Rest and Ice: Reducing activity and applying ice to decrease inflammation.
- Physical Therapy: Exercises to strengthen the calf muscles and improve flexibility. Eccentric strengthening exercises, which involve slowly lowering the heel after raising it, are particularly effective.
- Orthotics: Custom shoe inserts to support the foot and reduce strain on the tendon.
- Medications: Anti-inflammatory medications to relieve pain and swelling.
- Extracorporeal Shock Wave Therapy (ESWT): A non-invasive treatment that uses shock waves to stimulate healing in the Achilles tendon.
Surgical Treatments
In cases where non-surgical treatments are not effective, surgery may be necessary to repair the damaged tendon.
Surgical options include:
- Gastrocnemius Recession: This procedure involves lengthening the calf muscles to reduce stress on the Achilles tendon. It is particularly useful for patients with tight calf muscles².
- Debridement and Repair: If the tendon has significant damage, the surgeon may remove the damaged portion and repair the remaining healthy tendon. This procedure can be performed using open surgery or minimally invasive techniques.
- Tendon Transfer: In severe cases, a tendon transfer may be performed to replace the damaged Achilles tendon with another tendon from the foot.
- Minimally Invasive Surgery: Techniques that involve smaller incisions and less soft tissue disruption, leading to faster recovery times.
Risks and Benefits of Surgical Options
Gastrocnemius Recession
Benefits:
- Reduces stress on the Achilles tendon
- Improves flexibility and range of motion
Risks:
- Potential for nerve damage
- Possible infection or complications from anesthesia
Debridement and Repair
Benefits:
- Removes damaged tissue and promotes healing
- Can be performed using minimally invasive techniques
Risks:
- Risk of infection or nerve damage
- Longer recovery time compared to non-surgical treatments
Tendon Transfer
Benefits:
- Provides a durable solution for severe tendon damage
- Restores function and reduces pain
Risks:
- Potential for complications from the donor site
- Longer rehabilitation period
Prevention Tips
To prevent Achilles tendonitis, consider the following tips:
- Gradually increase the intensity of your workouts
- Stretch your calf muscles regularly
- Wear supportive footwear
- Avoid running on hard surfaces
Diabetic Wounds and Complications
What Are Diabetic Foot and Ankle Wounds?
Diabetic foot and ankle wounds, also known as diabetic ulcers, are open sores or wounds that commonly occur on the bottom of the foot. These ulcers are a significant complication of diabetes and can lead to severe consequences if not properly managed.
Why Are Diabetic Patients Prone to Foot and Ankle Wounds?
Diabetic patients are more prone to foot and ankle wounds due to several factors:
- Peripheral Neuropathy: High blood sugar levels can cause nerve damage, leading to a loss of sensation in the feet. This means that minor injuries or pressure points can go unnoticed and untreated, leading to ulcers.
- Poor Circulation: Diabetes can cause peripheral artery disease (PAD), which reduces blood flow to the extremities. Poor circulation impairs the body's ability to heal wounds and fight infections.
- Immune System Impairment: Diabetes can weaken the immune system, making it harder for the body to fight off infections.
The Role of Calluses in Developing Severe Complications
Calluses are thickened areas of skin that develop due to repeated friction or pressure. While they are generally harmless in healthy individuals, they can pose significant risks for diabetic patients:
Pressure Points: Calluses can create pressure points on the foot, leading to underlying tissue damage.
Cracking and Ulceration: Thick calluses can crack, providing an entry point for bacteria and leading to infections and ulcers.
Hidden Wounds: Due to neuropathy, diabetic patients may not feel the pain associated with calluses, allowing them to worsen unnoticed.
Impact on People's Lives
Diabetic foot and ankle wounds can significantly affect a person's quality of life. They can lead to chronic pain, reduced mobility, and in severe cases, amputation. The emotional and psychological toll can also be substantial, as patients may experience anxiety, depression, and a decreased ability to participate in daily activities.
Statistics on Diabetic Foot Wounds in the USA
Prevalence: About 15% of people with diabetes will develop a foot ulcer at some point in their lives.
Amputation Risk: Approximately 20% of people with diabetic foot ulcers will require an amputation.
Mortality Rate: The 5-year mortality rate for patients with a diabetic foot ulcer is between 50% and 70%.
Deformity and Risk
Diabetic patients are at risk of developing foot deformities due to neuropathy and poor circulation. Common deformities include:
Hammertoes: A condition where the toes are permanently bent.
Bunions: A bony bump that forms on the joint at the base of the big toe.
Charcot Foot: A severe deformity that occurs when the bones in the foot weaken and fracture, leading to changes in the shape of the foot.
Charcot Neuroarthropathy
Definition: Charcot neuroarthropathy, or Charcot foot, is a condition characterized by the weakening of the bones in the foot due to significant nerve damage. This can lead to fractures and dislocations, causing the foot to change shape.
Impact: Charcot foot can lead to severe deformities, making it difficult to walk and increasing the risk of ulcers and infections. If not treated promptly, it can result in amputation.
Prevention and Treatment
Prevention:
- Regular Foot Exams: Diabetic patients should have their feet examined regularly by a healthcare professional.
- Proper Footwear: Wearing well-fitting shoes that provide support and protection.
- Blood Sugar Control: Maintaining good blood sugar levels to prevent nerve and blood vessel damage.
- Daily Foot Care: Inspecting feet daily for cuts, blisters, or other injuries.
Treatment:
- Wound Care: Cleaning and dressing the wound to prevent infection.
- Offloading: Reducing pressure on the affected area using special footwear or casts.
- Medications: Antibiotics to treat infections.
- Surgery: In severe cases, surgery may be required to remove infected tissue or correct deformities.
The Importance of Podiatric Care
Podiatrists play a crucial role in identifying and preventing serious foot problems in diabetic patients:
- Early Detection: Regular check-ups with a podiatrist can help detect calluses, ulcers, and other issues before they become severe.
- Preventive Care: Podiatrists can provide guidance on proper foot care, footwear, and orthotics to prevent complications.
- Specialized Treatment: Podiatrists are trained to manage and treat diabetic foot conditions, reducing the risk of severe complications and improving overall foot health.
Diabetic foot and ankle wounds are a serious complication of diabetes that require prompt management. At BlueRock Podiatry, we are committed to providing comprehensive care to prevent and treat these wounds, helping our patients maintain mobility and quality of life.
Foot Surgery
Why Choose a Board-Certified Foot and Ankle Surgeon?
When it comes to foot and ankle surgery, choosing a board-certified surgeon ensures that you are receiving the highest standard of care. Board certification by the American Board of Foot and Ankle Surgery (ABFAS) signifies that the surgeon has undergone rigorous training and has demonstrated expertise in the field of foot and ankle surgery.
What is ABFAS Certification?
The American Board of Foot and Ankle Surgery (ABFAS) is the only certifying board recognized by the Council on Podiatric Medical Education (CPME) for foot and ankle surgery.
High Standards of Care
ABFAS certification requires surgeons to adhere to the highest standards of patient care. This includes maintaining up-to-date knowledge of the latest surgical techniques and best practices, ensuring that patients receive the most effective and safest treatments available.
Improved Outcomes
Studies have shown that patients treated by board-certified surgeons often experience better outcomes, including reduced complication rates and faster recovery times. This is because board-certified surgeons have the specialized skills and knowledge necessary to perform surgeries with precision and care.
Recovery Process After Foot Surgery
Recovering from foot surgery involves several stages, and the process can vary depending on the type of surgery performed.
Why Choose BlueRock Podiatry?
At BlueRock Podiatry, Dr. Jason Rockwood is a board-certified foot and ankle surgeon with extensive training and experience. Dr. Rockwood's commitment to excellence and patient-centered care ensures that you receive the highest quality treatment for your foot and ankle needs.
Contact Us
If you need foot or ankle surgery, don't settle for anything less than the best. Contact BlueRock Podiatry today to schedule an appointment with Dr. Jason Rockwood, a board-certified foot and ankle surgeon, and take the first step towards a successful recovery.
Wound Care
Diabetic Wounds and Complications of
the Foot and Ankle
What Are Diabetic Foot and Ankle Wounds?
Diabetic foot and ankle wounds, also known as diabetic ulcers, are open sores or
wounds that commonly occur on the bottom of the foot. These ulcers are a significant complication of diabetes and can lead to severe consequences if not properly managed.
Why Are Diabetic Patients Prone to Foot and Ankle Wounds?
Diabetic patients are more prone to foot and ankle wounds due to several factors:
1. Peripheral Neuropathy: High blood sugar levels can cause nerve damage, leading to a loss of sensation in the feet. This means that minor injuries or pressure points can go unnoticed and untreated, leading to ulcers.
2. Poor Circulation: Diabetes can cause peripheral artery disease (PAD), which
reduces blood flow to the extremities. Poor circulation impairs the body's ability to heal wounds and fight infections.
3. Immune System Impairment: Diabetes can weaken the immune system, making it harder for the body to fight off infections.
The Role of Calluses in Developing Severe
Complications
Calluses are thickened areas of skin that develop due to repeated friction or pressure.
While they are generally harmless in healthy individuals, they can pose significant risks
for diabetic patients:
Pressure Points: Calluses can create pressure points on the foot, leading to
underlying tissue damage.
Cracking and Ulceration: Thick calluses can crack, providing an entry point for
bacteria and leading to infections and ulcers.
Hidden Wounds: Due to neuropathy, diabetic patients may not feel the pain
associated with calluses, allowing them to worsen unnoticed.
Impact on People's Lives
Diabetic foot and ankle wounds can significantly affect a person's quality of life. They can lead to chronic pain, reduced mobility, and in severe cases, amputation. The
emotional and psychological toll can also be substantial, as patients may experience
anxiety, depression, and a decreased ability to participate in daily activities.
Statistics on Diabetic Foot Wounds in the USA
Prevalence: About 15% of people with diabetes will develop a foot ulcer at some
point in their lives.
Amputation Risk: Approximately 20% of people with diabetic foot ulcers will
require an amputation.
Mortality Rate: The 5-year mortality rate for patients with a diabetic foot ulcer is
between 50% and 70%.
Deformity and Risk
Diabetic patients are at risk of developing foot deformities due to neuropathy and poor circulation. Common deformities include:
Hammertoes: A condition where the toes are permanently bent.
Bunions: A bony bump that forms on the joint at the base of the big toe.
Charcot Foot: A severe deformity that occurs when the bones in the foot weaken
and fracture, leading to changes in the shape of the foot.
Charcot Neuroarthropathy
Definition: Charcot neuroarthropathy, or Charcot foot, is a condition characterized by
the weakening of the bones in the foot due to significant nerve damage. This can lead to
fractures and dislocations, causing the foot to change shape.
Impact: Charcot foot can lead to severe deformities, making it difficult to walk and
increasing the risk of ulcers and infections. If not treated promptly, it can result in
amputation.
Prevention:
- Regular Foot Exams: Diabetic patients should have their feet examined regularly by a healthcare professional.
- Proper Footwear: Wearing well-fitting shoes that provide support and protection.
- Blood Sugar Control: Maintaining good blood sugar levels to prevent nerve and blood vessel damage.
- Daily Foot Care: Inspecting feet daily for cuts, blisters, or other injuries.
Treatment:
- Wound Care: Cleaning and dressing the wound to prevent infection.
- Offloading: Reducing pressure on the affected area using special footwear or casts.
- Medications: Antibiotics to treat infections.
- Surgery: In severe cases, surgery may be required to remove infected tissue or correct deformities.
The Importance of Podiatric Care
Podiatrists play a crucial role in identifying and preventing serious foot problems in diabetic patients:
- Early Detection: Regular check-ups with a podiatrist can help detect calluses, ulcers, and other issues before they become severe.
- Preventive Care: Podiatrists can provide guidance on proper foot care, footwear, and orthotics to prevent complications.
- Specialized Treatment: Podiatrists are trained to manage and treat diabetic foot conditions, reducing the risk of severe complications and improving overall foot health.
Diabetic foot and ankle wounds are a serious complication of diabetes that require prompt and effective management. At BlueRock Podiatry, we are committed to providing comprehensive care to prevent and treat these wounds, helping our patients maintain their mobility and quality of life.
Visit BlueRock Foot & Ankle Today

Visit Blue Rock Podiatry Today
Address
3152 N University Ave, Provo, UT 84604
Suite #120
Phone Number
801-356-0233
Hours
Monday - Friday
9:00am - 5:00pm



